GLP-1 Therapy for Obese Patients with Diabetes: A Revolutionary Treatment Approach
Managing obesity and diabetes has always been a daunting task for healthcare professionals. The dual burden of these chronic conditions can lead to a range of serious health complications, including cardiovascular disease, kidney damage, and increased risk of mortality. However, recent advancements in the field of glucagon-like peptide-1 (GLP-1) therapies have provided a beacon of hope for millions of patients worldwide.
A Lucid Understanding of GLP-1 Therapy
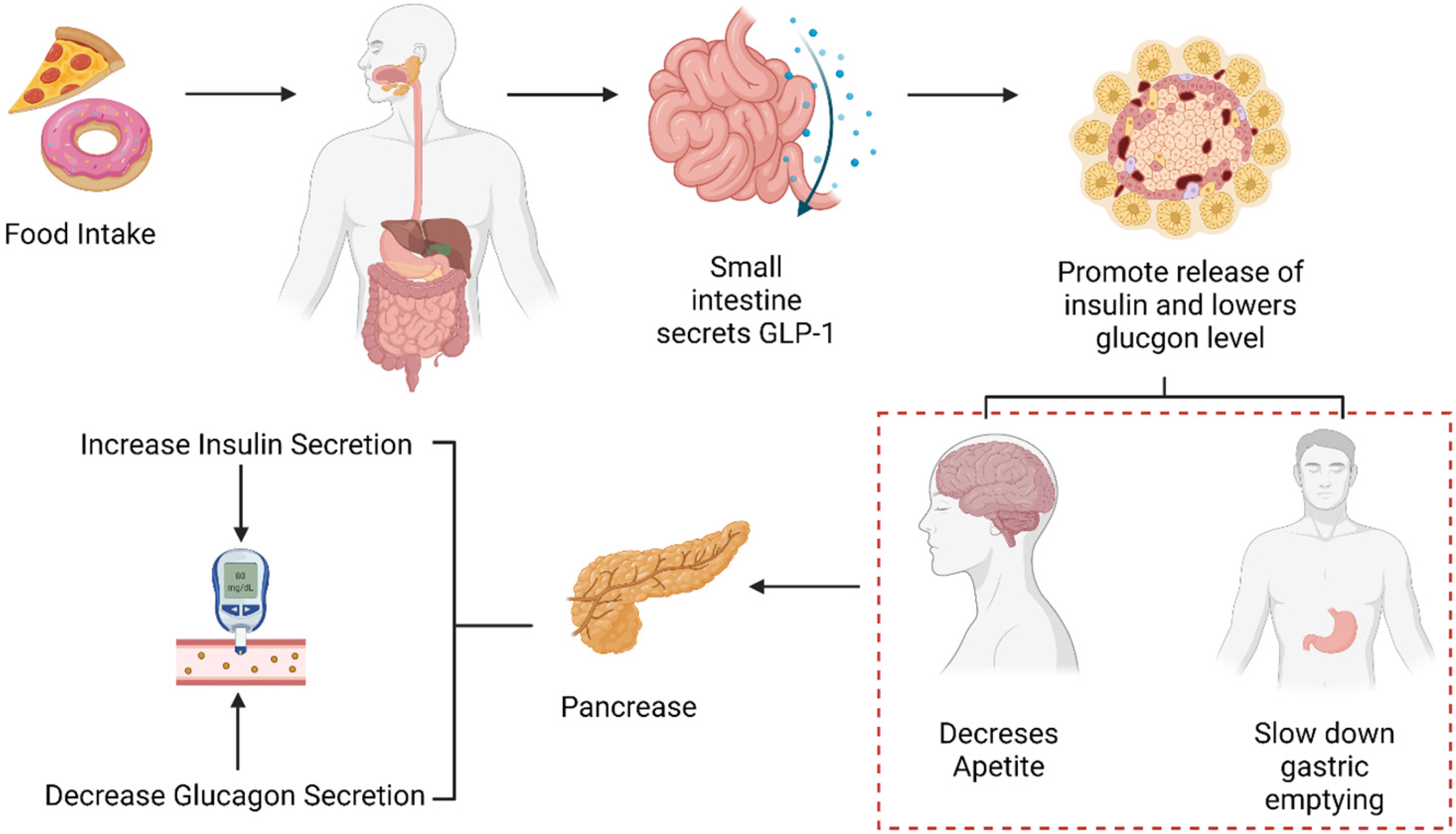
Developed as a treatment option for type 2 diabetes, GLP-1 therapies, including semaglutide and tirzepatide, have proven to be highly effective in controlling glucose levels and promoting weight loss. These medications work by mimicking the action of the incretin hormone GLP-1, which plays a crucial role in regulating blood sugar levels after a meal.
GLP-1 Therapy for Obesity: A Growing Area of Research
The WHO's recent guideline on the use of GLP-1 therapies for treating obesity as a chronic disease has sparked a surge in research and interest in this area. Studies have shown that GLP-1 therapies not only lead to significant weight loss but also reduce cardiovascular and renal morbidity and mortality. However, the use of these therapies poses clinical challenges, including loss of lean muscle mass and gastrointestinal side effects.
Benefits and Challenges of GLP-1 Therapy for Obese Patients with Diabetes
Regular use of GLP-1 therapies can have numerous benefits for obese patients with diabetes. These include:

- Improved weight loss and reduced body mass index (BMI)
- Enhanced glucose control, reducing the risk of hypoglycemia and diabetic complications
- Reduced cardiovascular risk and improved heart health
- Lower blood pressure and reduced risk of kidney damage
- Higher quality of life and increased self-esteem
However, challenges associated with GLP-1 therapy include:
- Loss of lean muscle mass, which can impact muscle strength and physical function
- Gastrointestinal side effects, such as nausea, vomiting, and diarrhea
- Increased risk of pancreatitis and pancreatolithiasis
- Dependence and withdrawal symptoms upon discontinuation
Case Study: GLP-1 Therapy for Obese Patients with Diabetes
A 45-year-old male patient with a BMI of 35 and type 2 diabetes was initiated on semaglutide therapy. Over a period of 6 months, he experienced a significant reduction in BMI and improved glucose control. Regular monitoring of his muscle mass and hemoglobin levels revealed no significant decline. However, he did experience side effects such as nausea and vomiting, which necessitated adjustments to his dosage and administration schedule.
Conclusion: Revolutionizing Diabetes and Obesity Management with GLP-1 Therapy
GLP-1 therapy represents a significant advancement in the management of diabetes and obesity. While challenges exist, the benefits of these therapies far outweigh the risks. Healthcare professionals and policymakers must work together to address these challenges and ensure widespread access to these life-changing treatments. By doing so, we can revolutionize diabetes and obesity management, leading to a healthier, happier global population.