GLP-1 and Blood Sugar Monitoring: A Comprehensive Guide
Understanding GLP-1
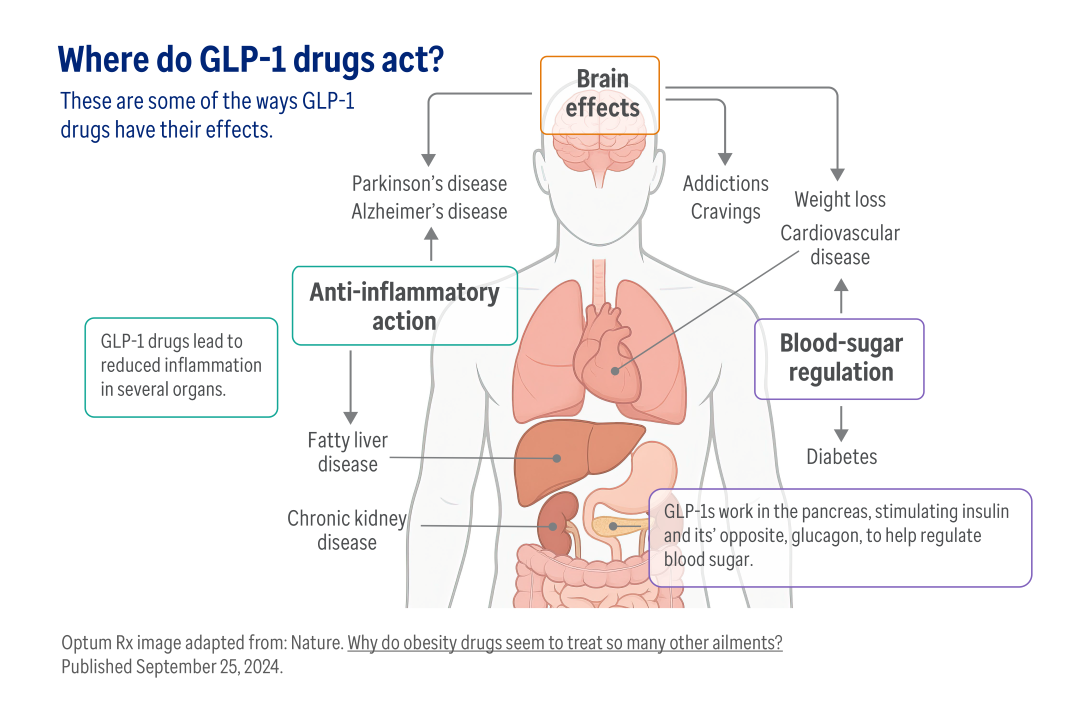
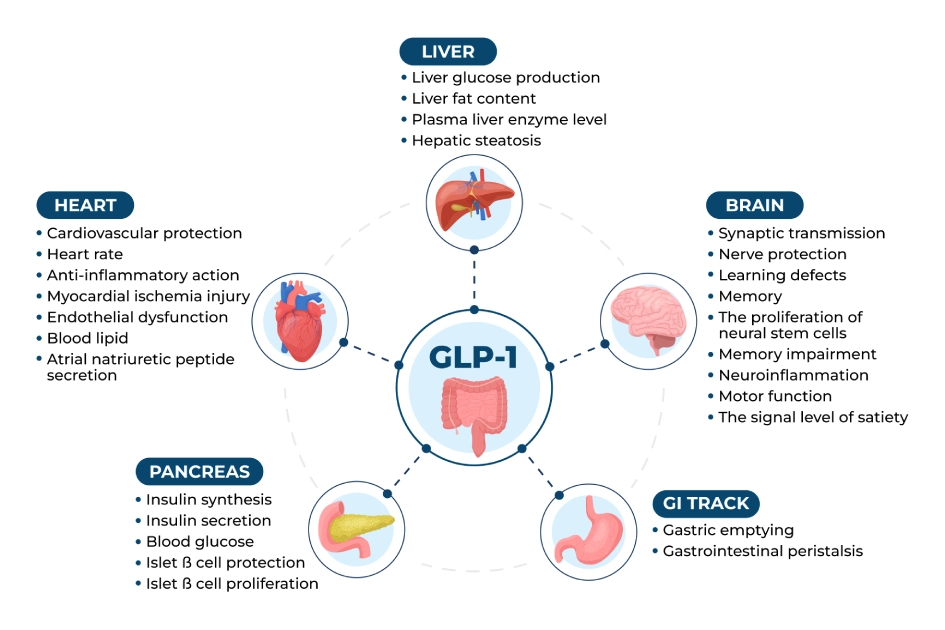
Glucagon-like peptide-1 (GLP-1) is a hormone produced in the intestines, primarily responsible for regulating blood sugar levels. GLP-1 stimulates the release of insulin, inhibits the release of glucagon, and slows gastric emptying. This complex mechanism helps to lower blood sugar levels and manage glucose metabolism.
Why GLP-1 Medications are Used to Monitor Blood Sugar

GLP-1 receptor agonists, such as semaglutide and tirzepatide, are designed to mimic the natural effects of GLP-1. These medications have become a popular choice for managing type 2 diabetes due to their ability to improve glycemic control, reduce appetite, and aid in weight loss. However, it's essential to use GLP-1 and blood sugar monitoring to ensure safe and effective treatment.
Lab monitoring is crucial when taking GLP-1 medications, especially for individuals with diabetes. As GLP-1 slows gastric emptying, it can lead to periods of low blood sugar, nausea, constipation, or dehydration. Close monitoring of blood sugar levels can prevent severe hypoglycemia, particularly when combined with insulin or sulfonylureas.
Essential Blood Tests for GLP-1 Medication Monitoring
- HbA1c: Monitoring HbA1c levels helps track long-term glycemic control and identifies potential signs of diabetes or prediabetes.
- Fasting Glucose: Regularly monitoring fasting glucose levels ensures that glycemic goals are being met and helps prevent hypoglycemia.
- Insulin Levels: Monitoring insulin levels helps identify changes in insulin sensitivity and adjust medication dosages as needed.
Why Lab Monitoring Matters on GLP-1 Therapy
GLP-1 medications often reduce appetite and slow gastric emptying, which can lead to periods of low intake, nausea, constipation, or dehydration. Close monitoring of blood glucose and lipid profiles can help prevent these complications and ensure the medication is working as intended.
The Importance of Self-Monitoring of Blood Glucose
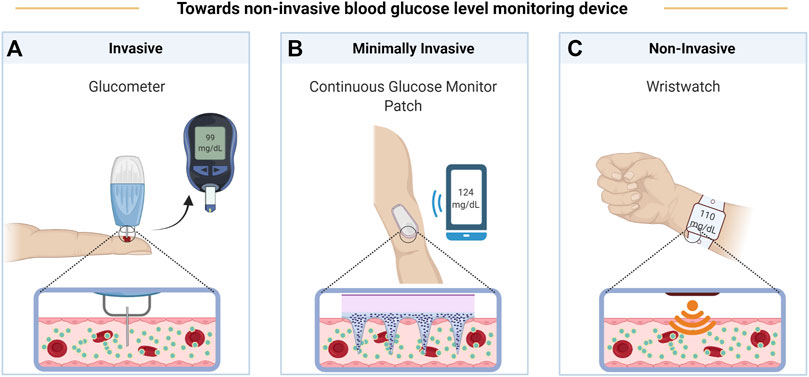
Self-monitoring of blood glucose remains a fundamental aspect of diabetes self-management, particularly for individuals treated with incretin-based drugs like GLP-1 receptor agonists. Continuous glucose monitoring systems and blood glucose meters are essential tools for monitoring glucose levels and adjusting treatment plans.
Discovering Side Effects with GLP-1 Therapy
As GLP-1 therapy can lead to various side effects, monitoring blood biomarkers can help identify changes in glucose metabolism, weight, and other related factors. Laboratory tests, such as kidney function and liver enzymes, are also important for ensuring medication safety and efficacy.
Recommended Testing Frequency and Accessible Lab Work
Regular monitoring of blood glucose and lipid profiles can help confirm that GLP-1 therapy is effective and adjust dosages as needed. For individuals interested in GLP-1 treatment, it is essential to discuss testing frequency and develop a plan for accessing affordable lab work with their healthcare provider.
Complete Guide to Lab Tests and Monitoring on GLP-1 Therapy
Getting started with GLP-1 therapy should include a comprehensive overview of recommended lab tests and monitoring. This guide should cover essential blood work, testing frequency, and result interpretation, allowing individuals to make informed decisions about their treatment plan.
Conclusion
GLP-1 and blood sugar monitoring are essential components of effective GLP-1 therapy, ensuring that blood sugar levels remain within a healthy range and preventing potential complications. Close monitoring of glucose levels and related factors allows healthcare providers to make informed decisions about medication adjustments and treatment plans, ultimately improving glycemic control and overall health outcomes.