Optimizing GLP-1 Receptor Agonist Dosing Schedule for Maximum Efficacy and Safety
Glucagon-like peptide-1 (GLP-1) receptor agonists are a class of medications that have revolutionized the management of type 2 diabetes and obesity. These agents mimic the natural hormone GLP-1, which plays a crucial role in regulating glucose and energy homeostasis. To maximize the efficacy and safety of GLP-1 receptor agonists, it is essential to understand the optimal dosing schedule.
The Importance of Gradual Dose Escalation
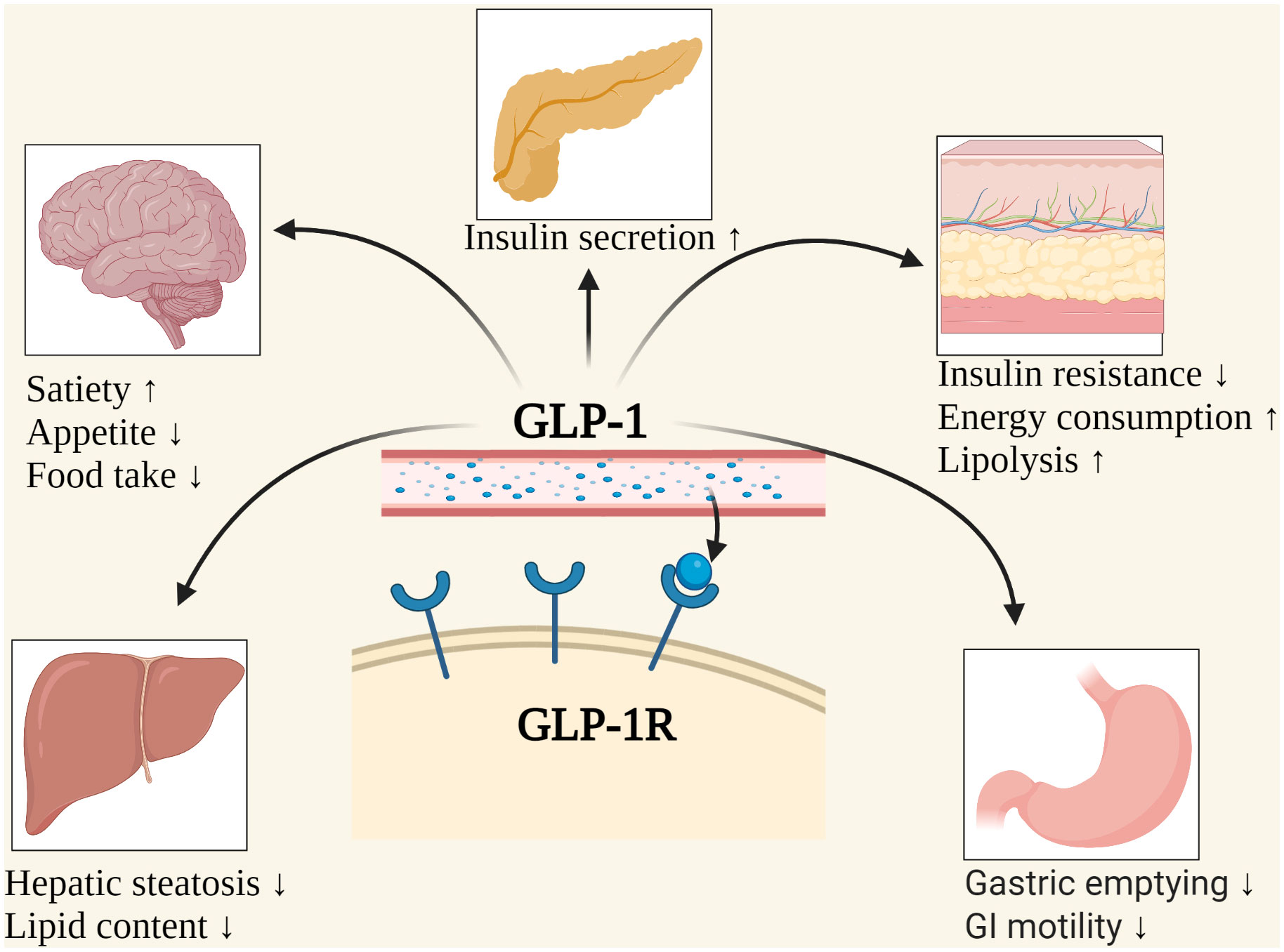
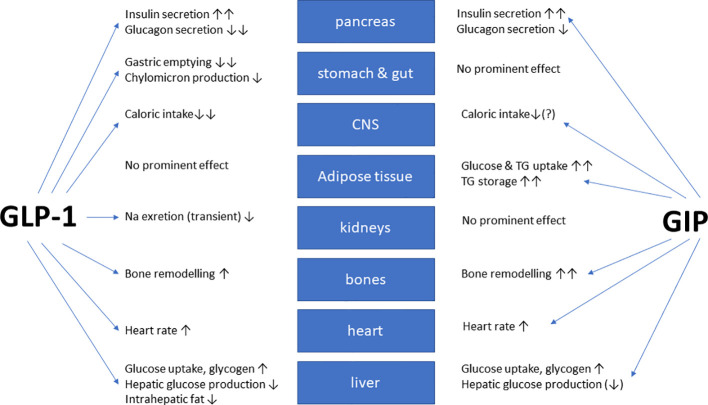
GLP-1 receptor agonists, such as semaglutide and liraglutide, work by slowing gastric emptying, acting on brain appetite centers, and reducing glucose levels. However, this increased activity can lead to gastrointestinal side effects, such as nausea, vomiting, and abdominal discomfort, which are the most common adverse events associated with these medications. To minimize these side effects, gradual dose escalation is crucial.
Understanding the GLP-1 Receptor Agonist Dosing Schedule
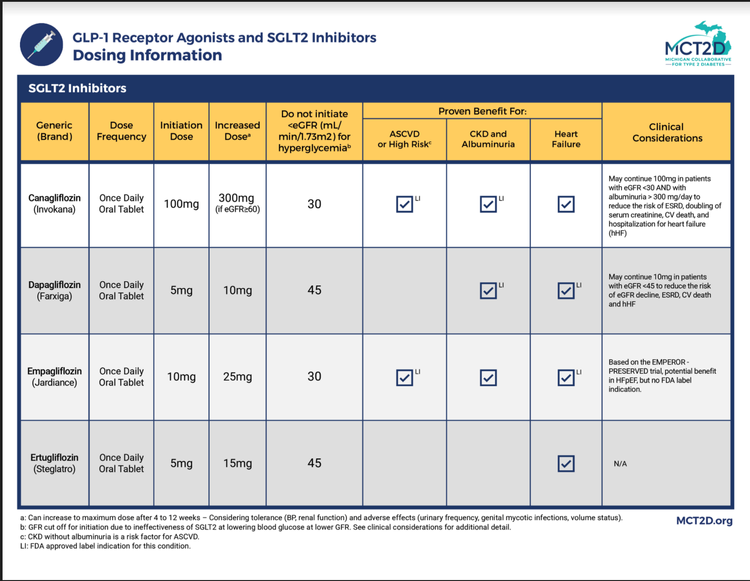
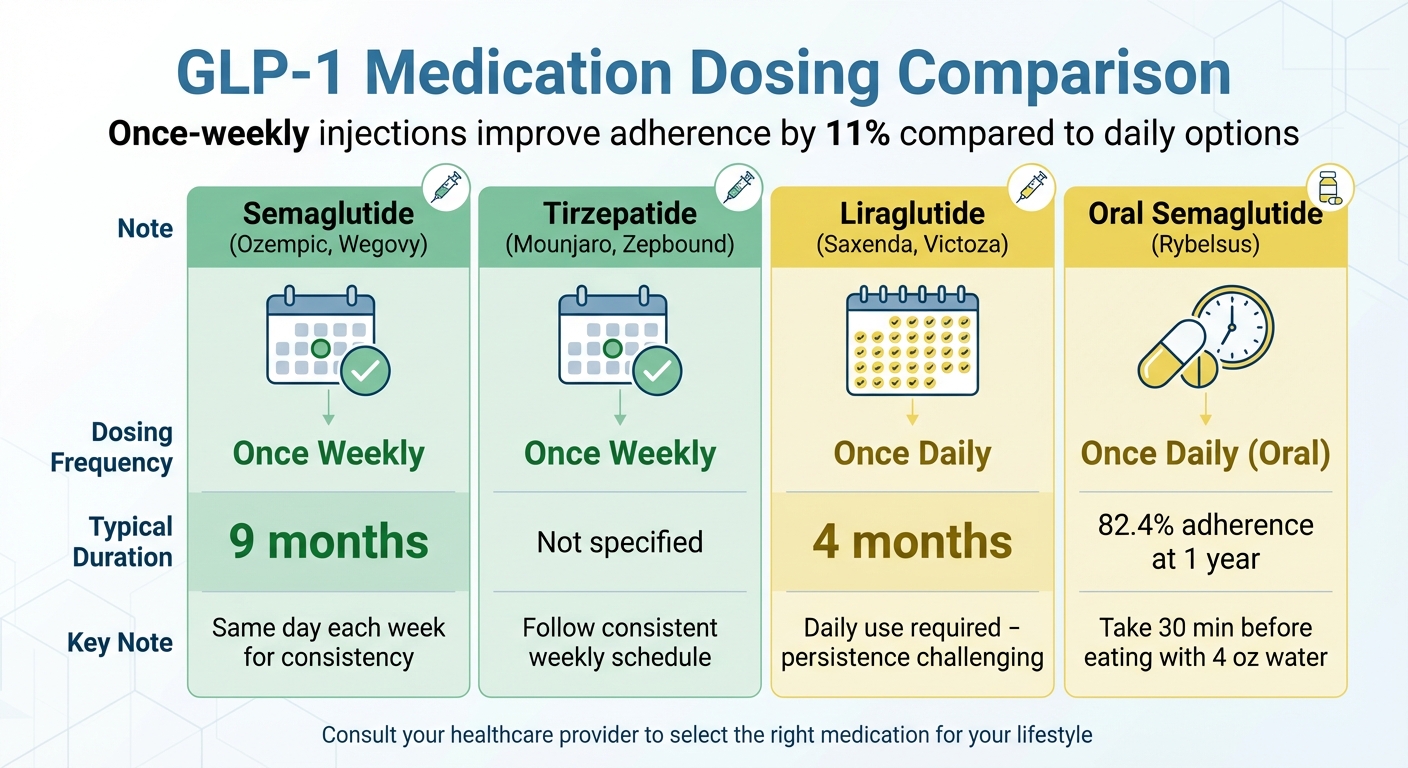
The dosing schedule for GLP-1 receptor agonists varies depending on the specific medication, treatment indication, and individual patient response. Some medications, such as semaglutide, are initiated at a lower dose and then gradually escalated to the maintenance dose. Others, such as liraglutide, may have a more rapid dose escalation schedule.
Key Considerations for Optimizing the GLP-1 Receptor Agonist Dosing Schedule
- Starting at a very low dose gives the digestive system time to adapt before the medication reaches full strength.
- Gradual dose escalation minimizes gastrointestinal side effects and allows the body to adapt to the medication.
- Individual responses to therapy may vary, and the dosing schedule may need to be adjusted accordingly.
- Monitoring of adverse effects, such as nausea and vomiting, is essential to optimize the dosing schedule.
- Adherence to the recommended dosing schedule is critical to ensure maximum efficacy and safety.
Examples of GLP-1 Receptor Agonist Dosing Schedules
Some examples of GLP-1 receptor agonist dosing schedules include:
Example 1: Semaglutide Dosing Schedule
- Initiate at 0.25 mg subcutaneously once weekly for 4 weeks.
- Increase to 0.5 mg subcutaneously once weekly for 4 weeks.
- Advance to the maintenance dose of 1 mg subcutaneously once weekly.
Example 2: Liraglutide Dosing Schedule
- Initiate at 0.6 mg subcutaneously once daily for 1 week.
- Increase to 1.2 mg subcutaneously once daily for 1 week.
- Advance to the maintenance dose of 1.8 mg subcutaneously once daily.
Conclusion
The GLP-1 receptor agonist dosing schedule plays a critical role in maximizing the efficacy and safety of these medications. By understanding the optimal dosing schedule, healthcare providers can minimize gastrointestinal side effects, improve adherence, and optimize patient outcomes. It is essential to monitor adverse effects, adjust the dosing schedule accordingly, and adhere to the recommended dosing regimen to ensure maximum efficacy and safety.
Recommendations
Based on the current evidence, the following recommendations can be made:
- Gradual dose escalation is essential to minimize gastrointestinal side effects and allow the body to adapt to the medication.
- Individual responses to therapy may vary, and the dosing schedule may need to be adjusted accordingly.
- Monitoring of adverse effects, such as nausea and vomiting, is essential to optimize the dosing schedule.
- Adherence to the recommended dosing schedule is critical to ensure maximum efficacy and safety.
Future Directions
Further research is needed to optimize the GLP-1 receptor agonist dosing schedule, taking into account individual patient responses, comorbidities, and potential interactions with other medications. Additionally, the development of new GLP-1 receptor agonists with improved safety and efficacy profiles may provide additional opportunities for optimization of the dosing schedule.