GLP-1 and Cardiovascular Disease Risk: Understanding the Connection
Glucagon-like peptide-1 receptor agonists (GLP-1RAs) have been a topic of interest in recent years, especially when it comes to managing diabetes and obesity. Research has shown that GLP-1 drugs can have a significant impact on cardiovascular disease risk, but how exactly do they work and what are the risks associated with stopping treatment? In this article, we'll explore the connection between GLP-1 and cardiovascular disease risk, including the benefits and potential drawbacks of using these medications.
What are GLP-1 Drugs?
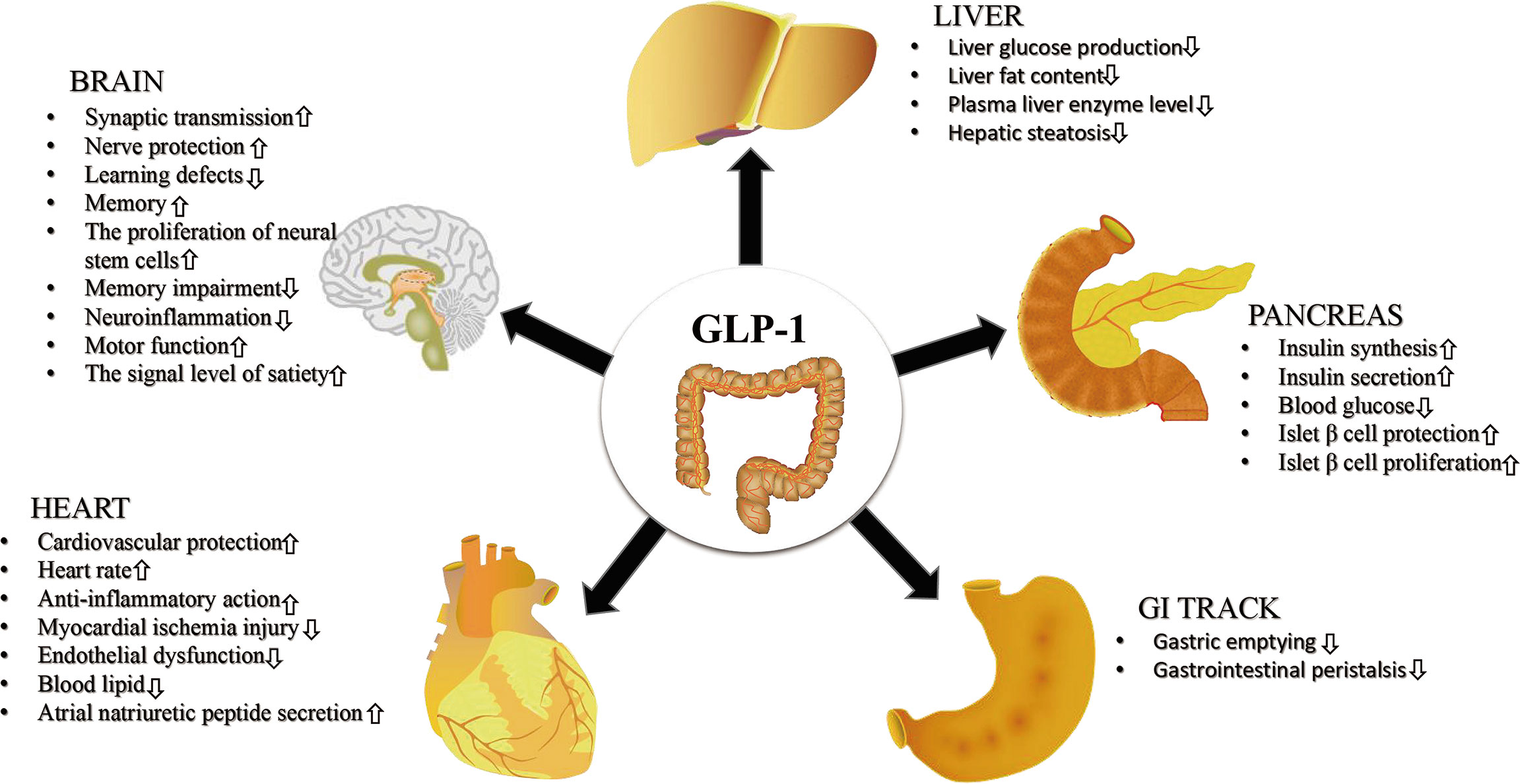
GLP-1RAs are a class of medications that mimic the action of the hormone glucagon-like peptide-1, which is released in response to meals. This hormone helps regulate blood sugar levels and suppresses the production of hunger hormones, leading to weight loss and improved glycemic control. Common GLP-1 drugs include semaglutide, tirzepatide, and liraglutide.
GLP-1 and Cardiovascular Disease Risk Reduction
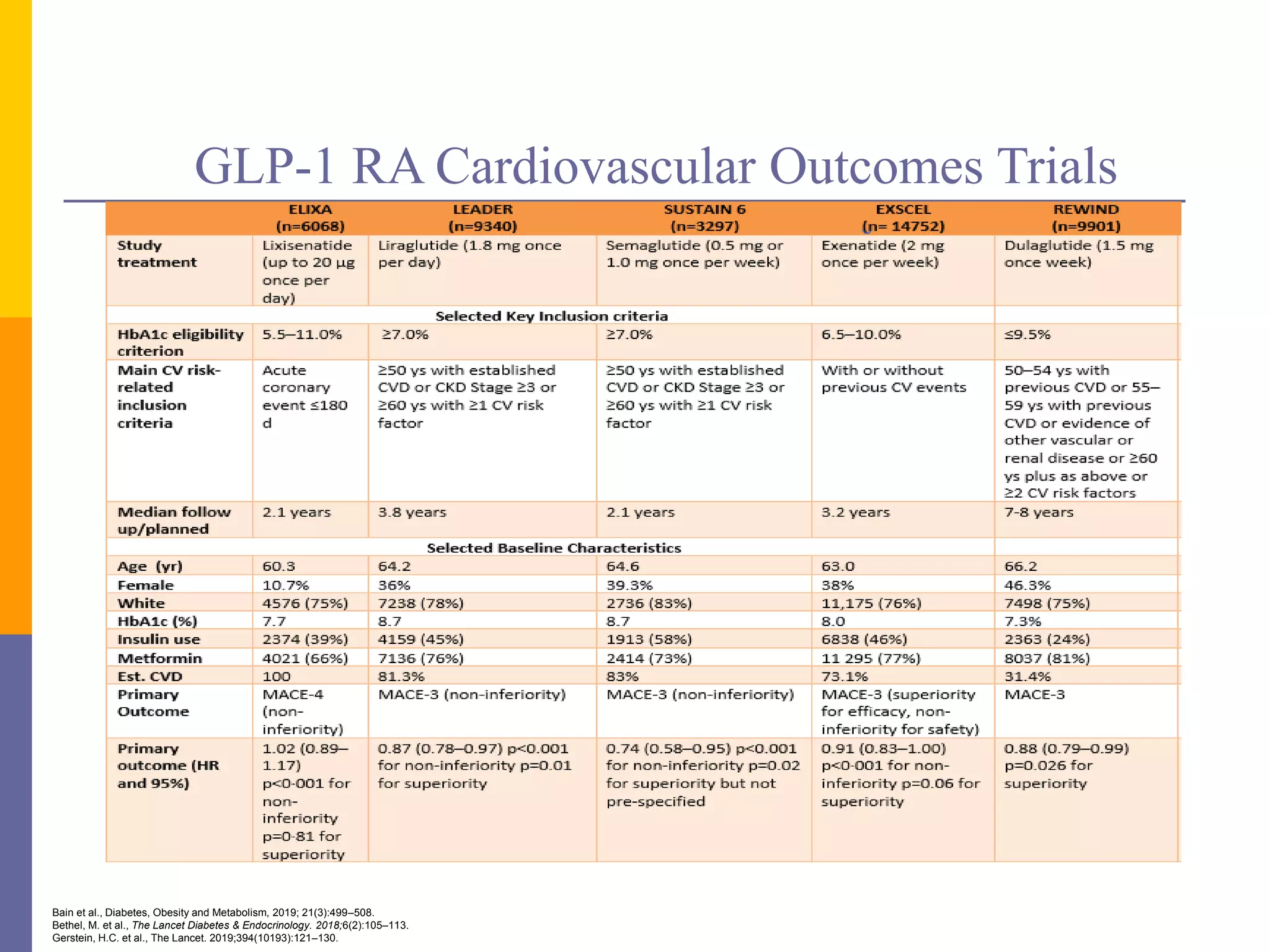
Research has consistently shown that GLP-1RAs can reduce the risk of major cardiovascular events, including heart attacks and strokes, in people with type 2 diabetes. A study published in BMJ Medicine found that continuous use of GLP-1 receptor agonists was associated with a lower risk of major cardiovascular events compared to sulfonylureas, with benefits increasing over time.
- A study of over 333,000 US veterans found that those who used GLP-1RAs and adhered to six to eight healthy habits had a 43% lower risk of serious cardiovascular events such as stroke and heart attack than those who didn't use the drugs and followed three or fewer such habits.
- A decade-long analysis of over 174,000 patients suggested that GLP-1 receptor agonists may reduce major cardiovascular events by 15% and end-stage kidney disease by 19% in type 1 diabetes.
GLP-1 and Cardiovascular Disease Risk Increases with Treatment Discontinuation
However, recent research has shown that stopping GLP-1 treatment can increase the risk of major cardiovascular events. A study found that even brief interruptions in treatment with GLP-1RAs can drive up the risk of heart attack, stroke, and death in patients with type 2 diabetes. Another study found that stopping or interrupting treatment for as little as six months was linked to a significant increase in the risk of major cardiovascular events.
- Stopping GLP-1 drugs like Ozempic can quickly erase cardiovascular benefits, with a 22% increase in cardiovascular risk after two years of not taking the medication.
- Research has shown that quitting GLP-1 drugs can reverse health gains and increase the risk of heart health risks.
Why is it Important to Understand GLP-1 and Cardiovascular Disease Risk?
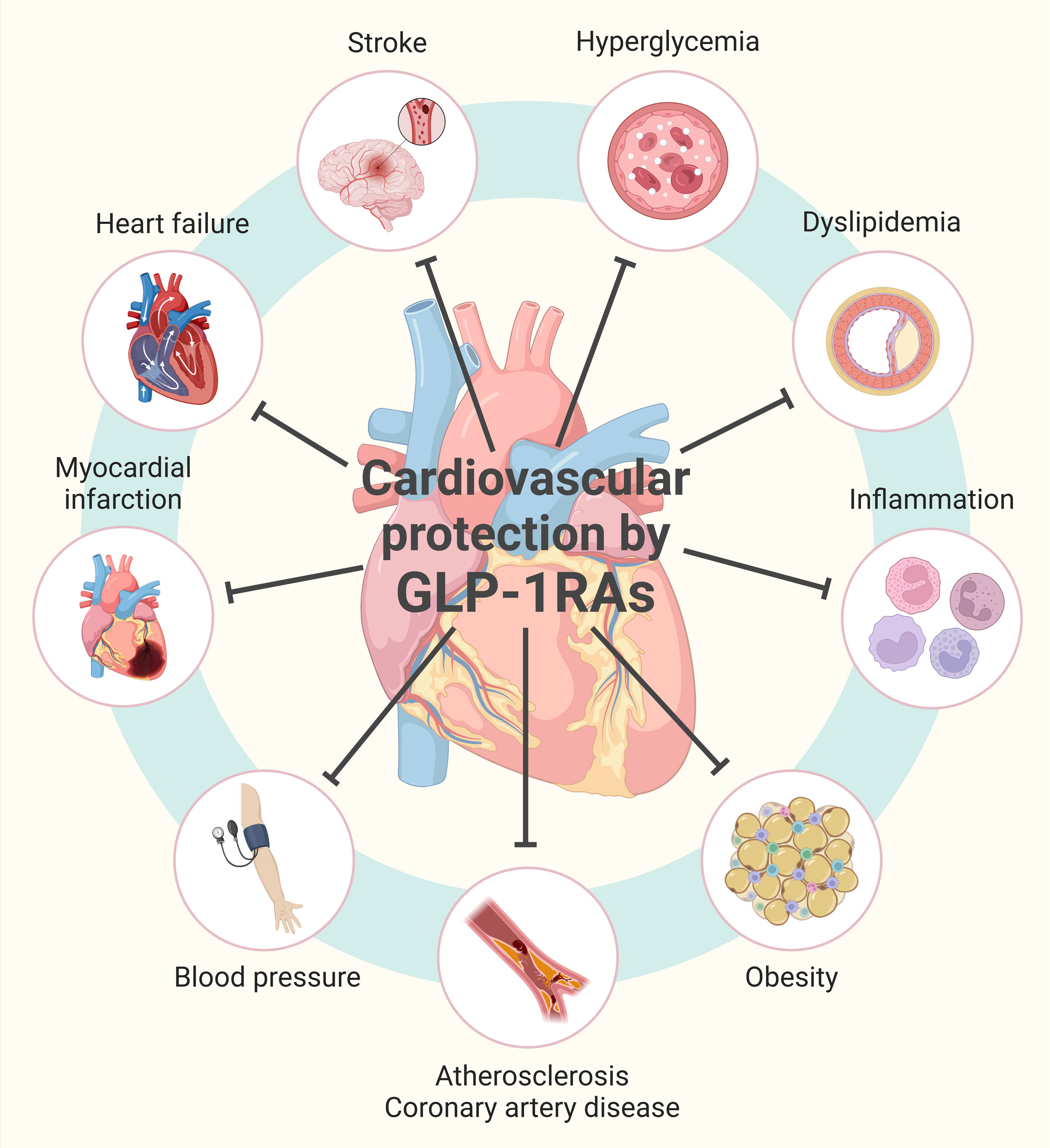
Understanding the connection between GLP-1 and cardiovascular disease risk is crucial for patients who are considering taking these medications. For individuals with existing heart disease or cardiovascular risk factors, a GLP-1 drug with proven cardiovascular benefits may be preferred. Additionally, research has shown that GLP-1RAs may have benefits beyond glycemic control, including reducing the risk of certain cancers, improving sleep apnea, and even dementia and addiction.
Conclusion
GLP-1RAs have been shown to have a significant impact on cardiovascular disease risk, with potential benefits including reduced risk of heart attack, stroke, and death. However, stopping treatment can increase the risk of major cardiovascular events. It's essential for patients to work closely with their medical team to weigh the benefits and risks of GLP-1RAs and to understand how they can effectively manage their cardiovascular health.
References
*Researchers at Washington University School of Medicine found that stopping GLP-1 drugs like Ozempic can lead to a significant spike in the risk of major cardiovascular events, with a 22% increase in risk for those who stop taking the drugs for one to two years.
*A study of over 174,000 patients suggested that GLP-1 receptor agonists may reduce major cardiovascular events by 15% and end-stage kidney disease by 19% in type 1 diabetes.