GLP-1 and Cardiovascular Disease Prevention in Diabetes
Glucagon-like peptide-1 (GLP-1) receptor agonists have revolutionized the treatment of type 2 diabetes (T2D) by not only improving glycemic control but also providing a range of cardiovascular benefits. These medications have been shown to reduce the risk of major adverse cardiovascular events (MACE) in patients with T2D, including heart attacks, strokes, and deaths. In this article, we will explore the role of GLP-1 in cardiovascular disease prevention in diabetes and discuss the latest research and clinical guidelines.
The Benefits of GLP-1 in Cardiovascular Disease Prevention
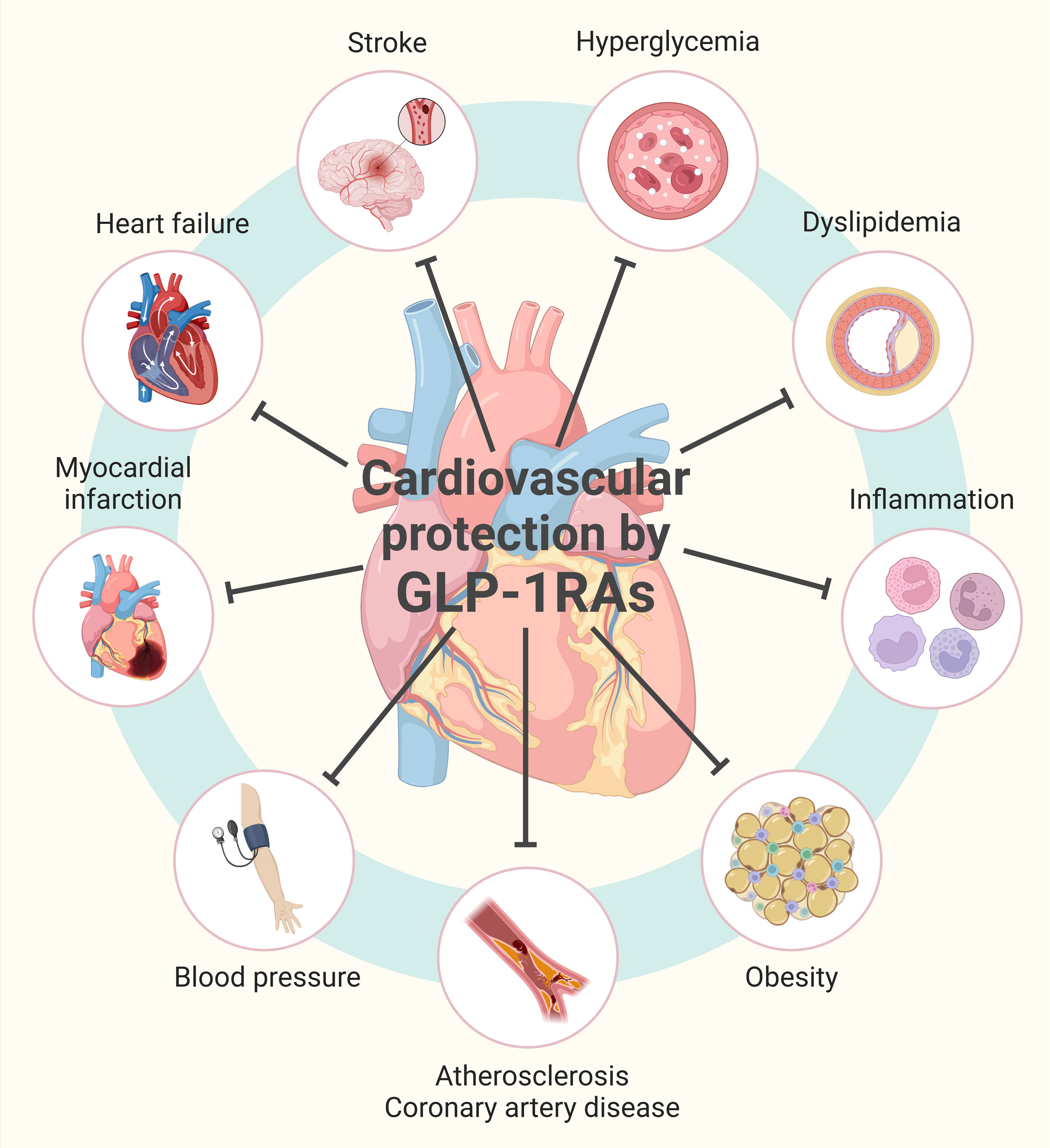
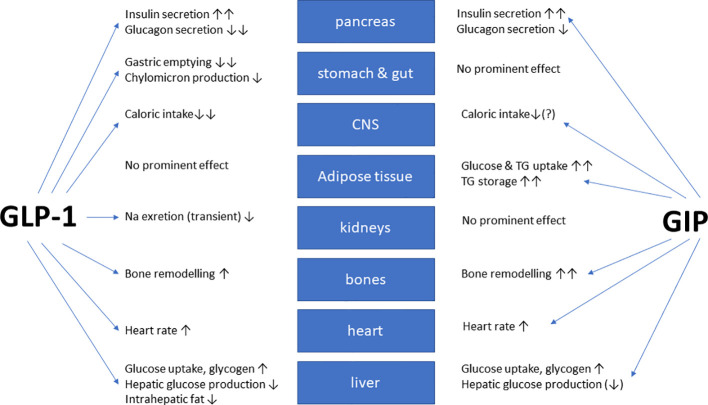
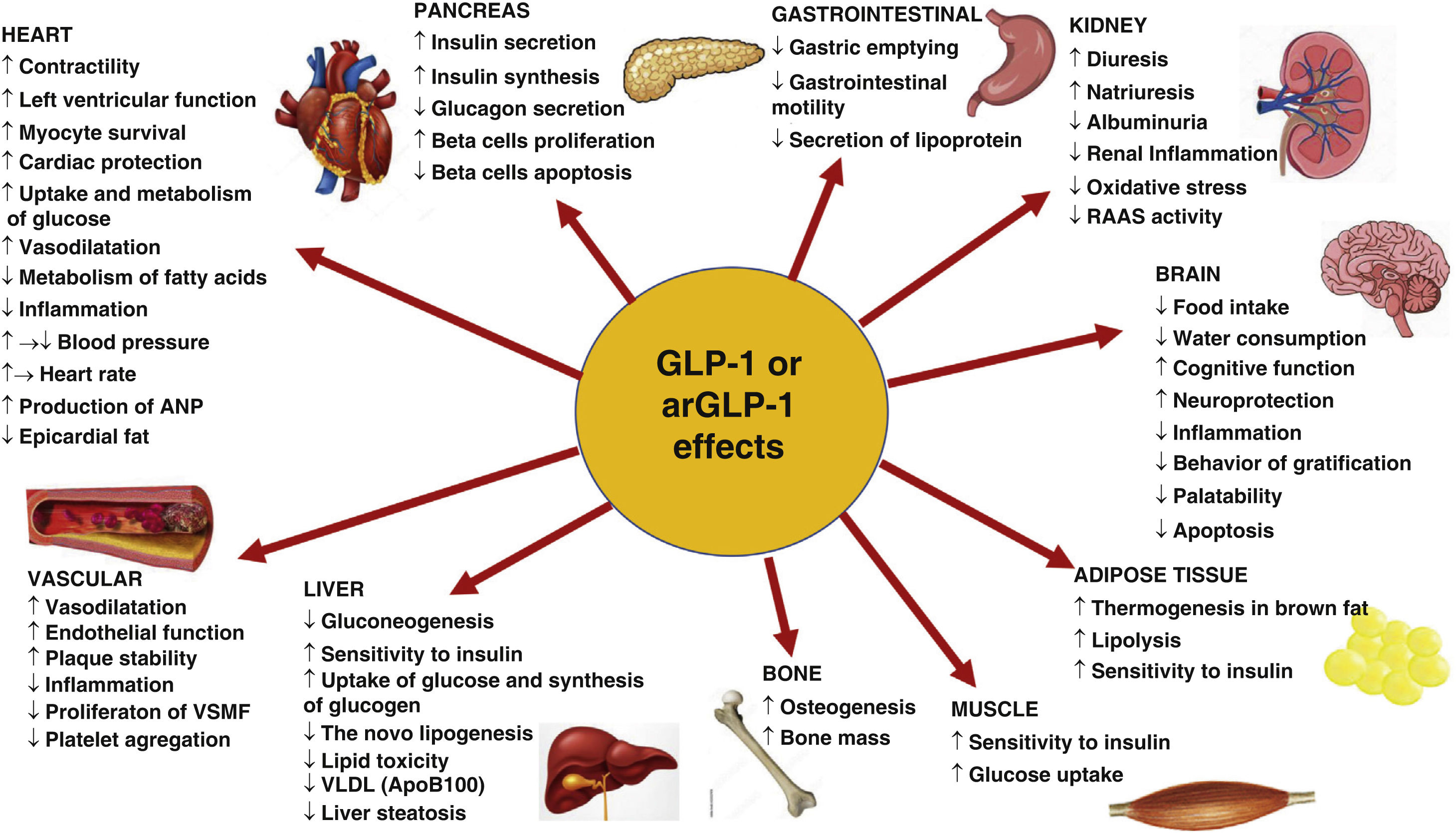
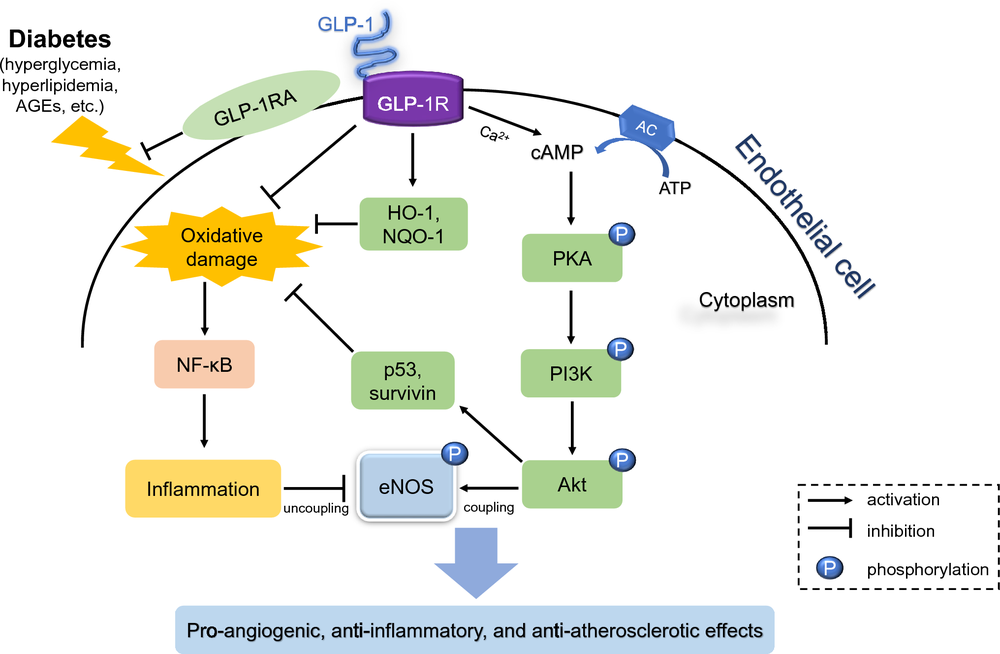
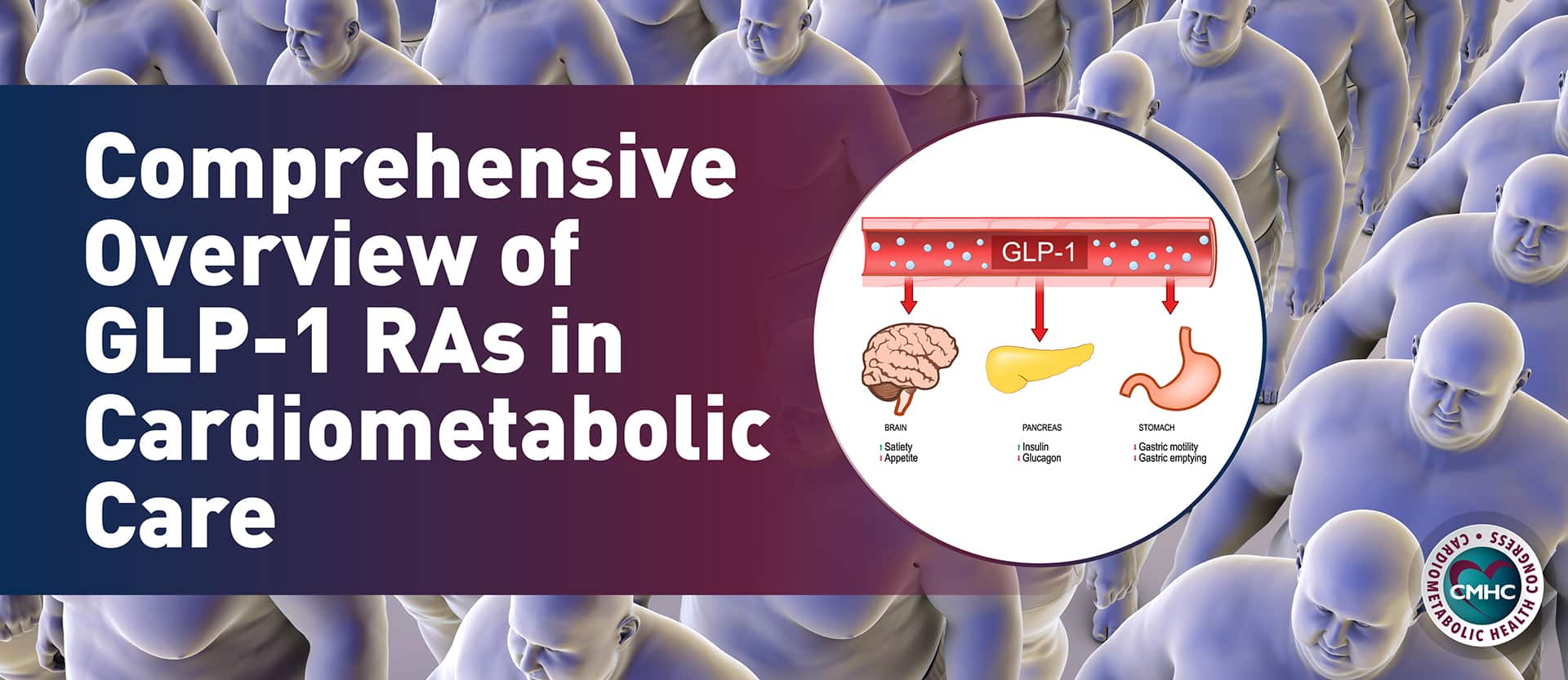
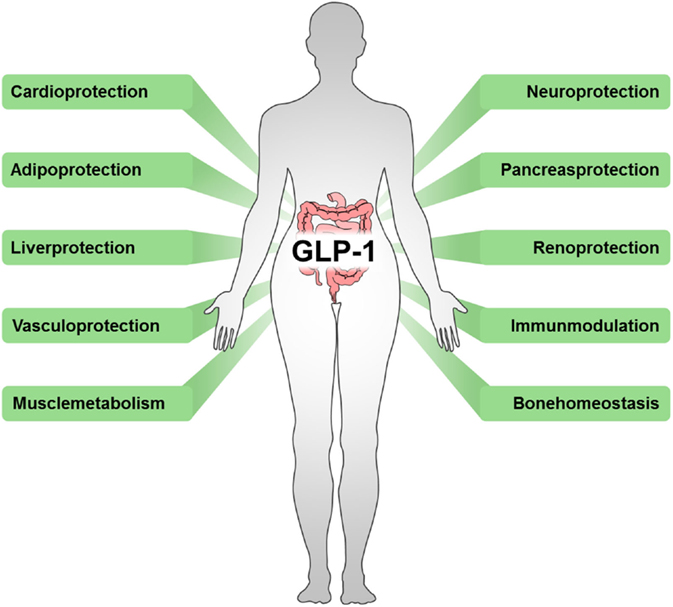
GLP-1 receptor agonists work by binding to GLP-1 receptors, which are widely distributed in the body, including cardiomyocytes and blood vessels. This binding action triggers a range of beneficial effects, including:
- Improved insulin sensitivity and glucose uptake
- Reduced blood pressure and cardiac output
- Improved lipid profiles and reduced inflammation
- Reduced renal dysfunction and fibrosis
These effects, combined with their ability to improve glycemic control, make GLP-1 receptor agonists a valuable addition to the treatment of T2D.
GLP-1 and Cardiovascular Disease Prevention in Clinical Trials
Multiple large cardiovascular outcome trials (CVOTs) have demonstrated the cardiovascular benefits of GLP-1 receptor agonists in patients with T2D. These trials have consistently shown that GLP-1 receptor agonists reduce the risk of MACE, including heart attacks, strokes, and deaths, in patients with T2D.
For example, the LEADER trial showed that liraglutide, a GLP-1 receptor agonist, reduced the risk of MACE by 13% compared to placebo in patients with T2D and established cardiovascular disease. Similarly, the SUSTAIN-6 trial demonstrated that semaglutide, another GLP-1 receptor agonist, reduced the risk of MACE by 26% compared to placebo in patients with T2D and established cardiovascular disease.
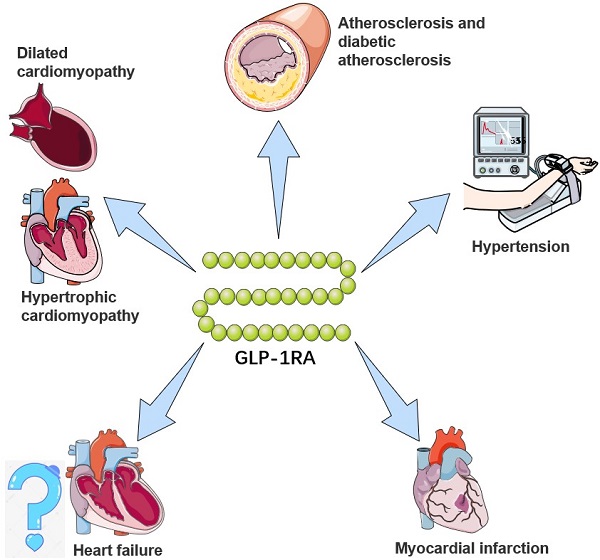
GLP-1 and Cardiovascular Disease Prevention in Clinical Practice
The cardiovascular benefits of GLP-1 receptor agonists have been consistently demonstrated in clinical trials, and these benefits are now reflected in clinical guidelines. For example, the American Diabetes Association (ADA) and the European Association for the Study of Diabetes (EASD) recommend the use of GLP-1 receptor agonists in patients with T2D and established cardiovascular disease to reduce the risk of MACE.
In addition to their cardiovascular benefits, GLP-1 receptor agonists also offer a range of other benefits, including weight loss, improved blood pressure, and reduced renal dysfunction. These benefits make GLP-1 receptor agonists an attractive option for patients with T2D and cardiovascular disease.
Conclusion
GLP-1 receptor agonists have revolutionized the treatment of T2D by providing a range of cardiovascular benefits. These medications have been consistently shown to reduce the risk of MACE in patients with T2D and established cardiovascular disease, and their use is now reflected in clinical guidelines. As our understanding of the cardiovascular benefits of GLP-1 receptor agonists continues to evolve, we can expect to see further improvements in the management and prevention of cardiovascular disease in patients with T2D.
References
This article is based on the following references:
- Abstract Glucagon-like peptide-1 (GLP-1) receptor agonists are well established drugs for the treatment of type 2 diabetes (T2D). In addition to glycemic control, GLP-1 receptor agonists have beneficial other effects.
- Jan 1, 2026Abstract Glucagon-like peptide-1 receptor agonists (GLP-1RAs) provide proven cardiovascular benefits in type 2 diabetes mellitus (T2DM) and heart failure, but their effects in patients with peripheral artery disease (PAD) remain unclear.
- Multiple large cardiovascular outcome trials with novel glucose-lowering agents, namely SGLT2i (SGLT2 inhibitors) and GLP-1RA (GLP-1 receptor agonists), have demonstrated robust and significant reductions of major adverse cardiovascular events (MACE) in patients with T2D and established cardiovascular disease.
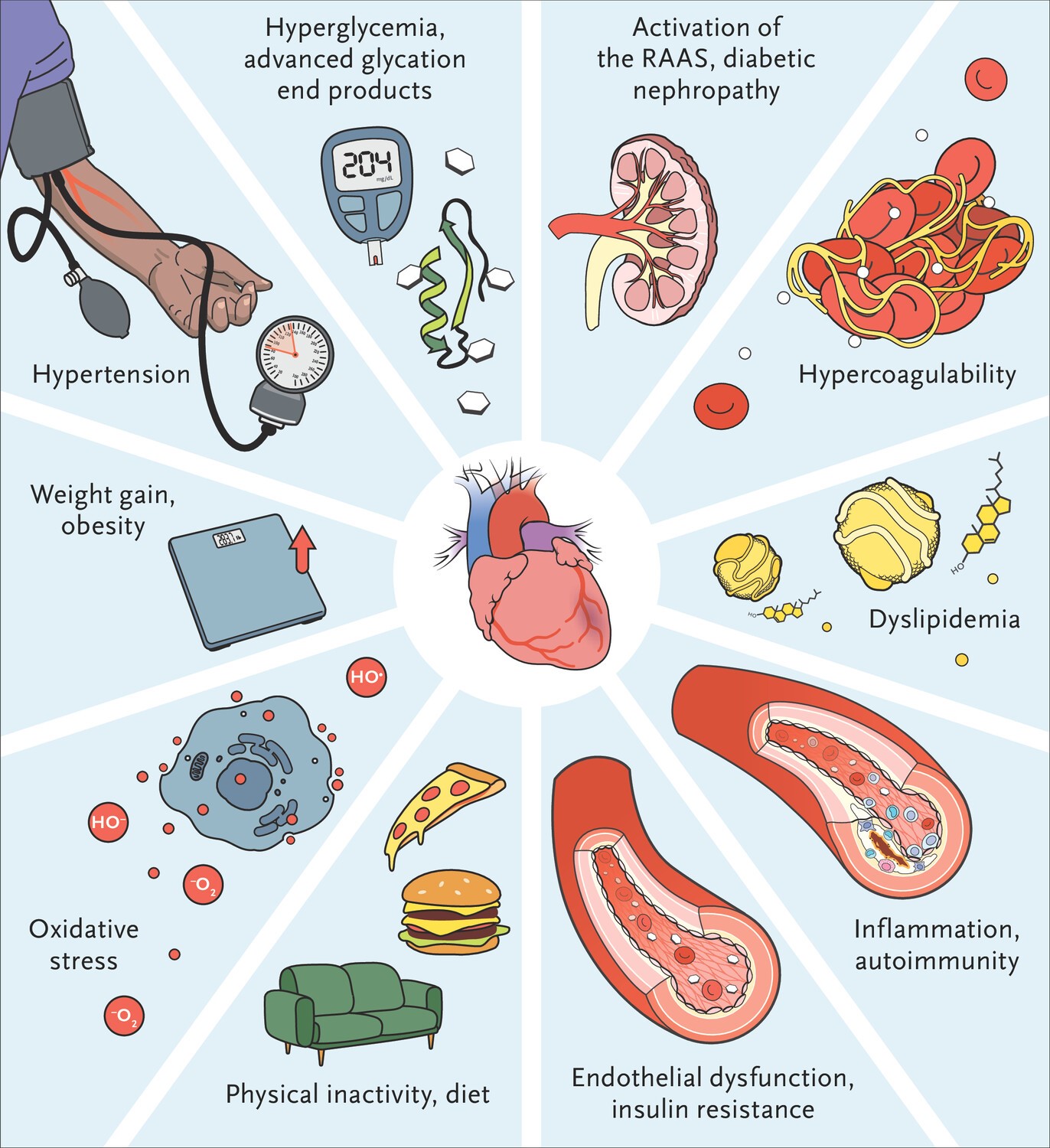
- Obesity and type 2 diabetes mellitus (DM) are among the most prevalent and rapidly increasing diseases worldwide. Both are major drivers of cardiovascular disease (CV) disease, which remains the leading cause of morbidity and mortality worldwide.
- Health care professionals should explore the use of glucagon-like peptide-1 receptor agonists (GLP1RAs) for cardiovascular risk reduction and their broader impacts on cardiometabolic health beyond diabetes mellitus management.
- Research finds that even short gaps in treatment with a GLP-1 can drive up risks of heart attack, stroke, and death in patients with Type 2 diabetes.
- GLP-1 drugs have moved far beyond their original role in type 2 diabetes care. These medications now play a central part in preventing and managing a wide range of cardiometabolic conditions, including heart disease, kidney disease, and obesity.
- This cohort study examines associations of glucagon-like peptide-1 receptor agonist (GLP-1RA) use with cardiovascular and kidney outcomes across body mass index (BMI) categories in patients with type 2 diabetes.
- A new study finds quitting GLP-1 drugs like Ozempic can reverse health gains and increase heart health risks.
- GLP-1RA medications are not FDA-approved for the prevention of Type 2 diabetes in people with prediabetes.
- The benefits attributed to glucagon-like peptide-1 (GLP-1) receptor agonists continue to accumulate. Initially developed to improve blood sugar control in individuals with type 2 diabetes, GLP-1 medications are among the most sought-after drug classes because of their weight-loss capabilities and positive effects on other cardiovascular disease (CVD) risk factors.
- A recent analysis reveals that stopping GLP-1 receptor agonist medications—a class of drugs increasingly used for both diabetes and weight management—can quickly erode the cardiovascular benefits they provide, potentially increasing the risk of heart attack, stroke, and even death.
- Clinicians are now prescribing GLP-1 receptor agonists for conditions that have nothing to do with weight loss or blood sugar control, and the list is growing fast.
- Learn more about how GLP-1 therapies are evolving beyond diabetes to support cardiovascular, kidney, and inflammatory health.
- GLP-1RA medications are not FDA-approved for the prevention of type 2 diabetes in people with prediabetes.
- Type 2 diabetes risk varies widely for adults 18-40 with prediabetes. High glucose and obesity significantly increase the 5-year progression risk to nearly 25%.
- Nearly half of all adults in the U.S. have high blood pressure (≥130/80 mm Hg), which is the #1 preventable risk factor for cardiovascular disease, including heart attack, stroke, and heart failure, as well as kidney disease.
- As outlined in more detail in section 9, "Pharmacologic Approaches to Glycemic Treatment," and section 10, "Cardiovascular Disease and Risk Management," the cardiovascular benefits of SGLT2 inhibitors or GLP-1RAs are not contingent upon A1C lowering; therefore, initiation should be considered in people with type 2 diabetes and CVD.
- Explore GLP-1 blood pressure effects and how these diabetes therapies improve vascular health, reduce hypertension, and support cardiometabolic outcomes.
- New stroke prevention guidelines recommend GLP-1 medications like Ozempic for those with type 2 diabetes or heart disease to lower stroke risk. Here's what to know.
- GLP-1RA and SGLT2 inhibitors remain foundational These agents are prioritized for both glycemic control and organ protection (heart, kidney, weight). Right diagnosis precedes right treatment AACE introduces emphasis on evaluating diabetes type—avoid mislabeling all patients as T2D.
- Lilly's Mounjaro (tirzepatide), a GIP/GLP-1 dual agonist, demonstrated cardiovascular protection in landmark head-to-head trial, reinforcing its benefit in patients with type 2 diabetes and heart disease.
- GLP-1RA medications are not FDA-approved for the prevention of Type 2 diabetes in people with prediabetes.